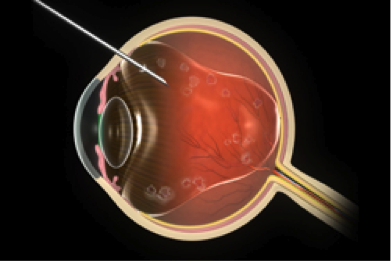
The researchers then conducted tests in mice by inciting in the mouse retina abnormal blood vessel growth similar to that seen in humans with macular degeneration. The researchers hypothesized this protein may help protect patients from developing wet AMD. They further observed that the levels of this protein were higher in patients who did not develop wet AMD compared with patients who did. The researchers found that apolipoprotein B100 was present at much higher levels in the eyes of patients who had been weaned off anti-VEGF treatment. In a proof-of concept experiment, the researchers chose one of the 172 proteins to investigate further - apolipoprotein B100 - that other studies had demonstrated is an important part of drusen, the material that accumulates under the retina in all patients with AMD and was thought to promote early changes in dry AMD. 
In the fluids, the researchers found differences in the amounts of 172 proteins between patients who were able to stop treatments compared with those who required monthly treatment. The researchers next sought biomarkers that could show what distinguished these patients from those who required monthly injections to maintain their vision.īefore beginning treatment with anti-VEGF therapy using their treatment plan, Sodhi’s team collected small amounts of fluid from the eyes of some of the patients, and continued collecting samples at subsequent clinic visits from many of the patients. They had better visual acuity, better gain of vision and less fluid in their retina,” says Sodhi. “Across the board, the patients who could enter a treatment pause did the best even though they were receiving no anti-VEGF drugs. 
Patients who stopped anti-VEGF treatments in at least one eye showed the best outcome, with less fluid and improved vision compared with those who required continued injections to maintain their vision. The other half of patients required treatment every 6–12 weeks a handful of these patients were also ultimately weaned from treatment at the end of year two. A smaller percentage of eyes still required monthly injections, amounting to treatments for 21 of 122 (17%) patients’ eyes. That amounted to 38 of 122 (31%) of treated eyes. Eyes without treatment that showed no signs of fluid accumulation or advancing vision loss after at least 30 weeks of monitoring were considered safely weaned off anti-VEGF therapy.Īt the end of a year, up to a third of the patients had stopped anti-VEGF treatments in at least one eye. However, the need to return to a physician’s office or clinic each month for injections is a common barrier to care among patients, leading to missed treatments and potentially worsening vision.įor the study, Sodhi and his team analyzed the treatment outcomes of 106 people with wet age-related macular degeneration whom he treated at the Johns Hopkins Wilmer Eye Institute between 20 at the East Baltimore location and at a satellite clinic, both in Maryland.Įach patient had undergone a customized anti-VEGF injection schedule in which Sodhi monitored response to therapy and determined whether patients needed another injection at each visit or if they could enter a treatment pause in which the injection was held unless there was evidence of new disease activity at the next visit. Anti-VEGF agents can slow or stop the growth of the leaky blood vessels and, in most cases, effectively stave off further vision loss. Treatment of wet AMD requires monthly or bimonthly injections of drugs called anti-VEGF - or anti-vascular endothelial growth factor - into the eye. The majority of those who lose vision from the condition have the “wet” form, characterized by the abnormal growth of blood vessels that leak damaging fluids into the light-sensitive tissues of the eye. 18 in the Journal of Clinical Investigation.Īge-related macular degeneration (AMD) is the most common cause of vision loss among people age 50 and older. “Such a test could let us tell patients early on how well they would do and when they might be able to stop,” says Akrit Sodhi, M.D., Ph.D., associate professor of ophthalmology and the Branna and Irving Sisenwein Professor of Ophthalmology at the Johns Hopkins University School of Medicine and Wilmer Eye Institute. The findings, the investigators say, also point to specific proteins produced at different levels in the eyes of those who stopped therapy, which may lead to the development of a test to accurately identify who may be weaned off medication.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
